3800 Reservoir Rd, 1st Floor Gorman
Washington, DC 20007
6862 Elm St, Suite 800B
McLean, VA 22101

3800 Reservoir Rd, 1st Floor Gorman
Washington, DC 20007
6862 Elm St, Suite 800B
McLean, VA 22101
Message Sent!
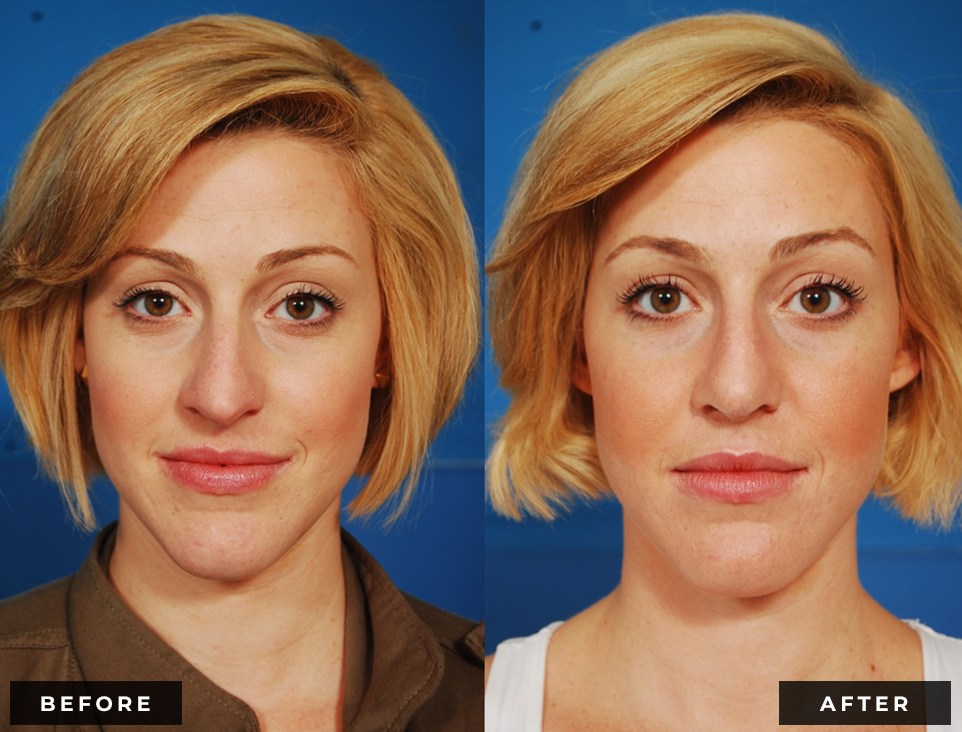
Rhinoplasty, commonly known as a “nose job,” is a surgical procedure designed to enhance the shape, structure, and function of the nose. This procedure can address both cosmetic concerns and functional issues, such as breathing difficulties.
A thorough clinical evaluation is essential for determining the best surgical approach. During your consultation, Dr. Reilly will assess your nasal anatomy and discuss your goals. A customized surgical plan will be developed to ensure that your desired results align with the most appropriate treatment options. Learn more about our Rhinoplasty pricing information.
While rhinoplasty is generally an elective procedure, it can provide significant aesthetic and functional benefits. In addition to improving nasal appearance, surgery can help enhance breathing by correcting structural issues.
The procedure involves making incisions inside the nostrils, with or without an additional incision on the columella (the small strip of tissue between the nostrils). These incisions provide access to reshape the underlying nasal structures, ensuring a balanced and harmonious result.
Most patients take one week off work, followed by another week of reduced activity. After 2 weeks, you may resume full activity except contact sports, which must be avoided for 6 weeks.
A rhinoplasty, or “nose job,” is a surgical procedure that is performed by an ENT or facial plastic surgeon to alter your nasal anatomy. This can be done for cosmetic reasons, functional reasons, or both. Even for patients who have no symptoms of nasal obstruction, rhinoplasty surgery should always incorporate a plan for maintaining the optimal breathing function of your nose.
During your initial consultation, Dr. Reilly will perform an in-depth examination of your nose. You and he will discuss, in detail, your desired cosmetic and/or functional outcome. During the cosmetic consultation, Dr. Reilly will take photos of you and use editing software to help mutually determine a realistic plan for your rhinoplasty surgery with you.
Dr. Reilly is known for his natural looking results, and he is passionate about providing his patients with the best possible outcomes.
The short answer is that, for safety reasons, I generally do not recommend liquid rhinoplasty. Although certainly less invasive than a surgical rhinoplasty, filler injections come with an uncommon but major risk called injection related vascular compromise or IRVC. Injecting the filler material into or around a blood vessel can lead to diminished blood flow to the tissue. In rare instances, the filler can move through the small vessels of the face back toward the eye and can result in blindness.
A “functional rhinoplasty” is surgery that focuses on optimizing the structure of the nose to improve breathing. While there may be some mild changes in nasal appearance that occur whenever the structure of the nose is manipulated, this procedure is not done for cosmetic reasons. Most insurance providers have strict guidelines for covering procedures such as this.
Procedures that are cosmetic in nature are not covered by insurance companies. My rhinoplasty surgeon’s fees range from $6,000 (small changes to the nasal tip only) to $15,000 (complex revision rhinoplasty), with the average fee being $10,000. The total price for my rhinoplasty surgeries (including surgeon’s, anesthesia, and operating room fees) ranges from $8.200 for a tip rhinoplasty requiring one hour to $21,000 for a complex revision rhinoplasty requiring four hours. The average of cost of a purely cosmetic rhinoplasty is about $15,000 depending on the degree of intervention desired and the corresponding duration of time required to accomplish my patient’s goals. After your consultation with Dr. Reilly, you will be provided a personalized quote based on the scope of work discussed. Any functional surgery aimed at improving breathing or correcting a traumatic or congenital deformity is considered separate from the cosmetic surgery and will be submitted to your insurance for authorization. Dr. Reilly performs surgery out of MedStar Georgetown University Hospital, which offers competitive pricing for the anesthesia fee and operating room charges. We have a team who will help navigate you through this process.
Surgical rhinoplasties are essentially permanent, but they do not stop the aging process. Noses over time have a tendency to droop. They aren’t growing, but the support tissues that keep things tight start to become lax, which causes spreading and drooping of the nasal support. Pesky gravity. A rhinoplasty can decrease the drooping process to some degree because of structural reinforcement and scar tissue that helps mitigate this tissue loosening and the resulting downward tissue movement.
My rhinoplasty surgeon’s fees range from $6,000 (small changes to the nasal tip only) to $15,000 (complex revision rhinoplasty), with the average surgical fee being $10,000. The total price for my rhinoplasty surgeries (including surgeon’s, anesthesia, and operating room fees) ranges from $8,200 for a tip rhinoplasty requiring 1 hour to $21,000 for a complex revision rhinoplasty requiring 4 hours. Learn more.
Understanding Rhinoplasty
Rhinoplasty, commonly referred to as a “nose job,” is one of the most frequently performed plastic surgeries in the United States. Since the nose plays a central role in facial symmetry, its size and shape can significantly impact one’s appearance and confidence.
This procedure is performed for various reasons, including:
Rhinoplasty is designed to improve both the aesthetic and functional aspects of the nose. The procedure involves making incisions inside the nostrils, with or without an additional incision on the columella (the small strip of tissue between the nostrils). In some cases, cartilage from the ear may be needed for reconstruction, requiring a minor incision in the outer ear.
Although rhinoplasty is typically an elective procedure, it can enhance facial balance and improve breathing. While most patients achieve their desired results, potential risks include:
Insurance Coverage: Cosmetic rhinoplasty is generally not covered by insurance. However, procedures aimed at improving nasal function or correcting traumatic deformities may qualify for partial or full coverage. Our team will assist you in determining your insurance eligibility.
The surgery begins by accessing the underlying bone and cartilage through strategic incisions inside the nostrils and, in some cases, along the columella. The nasal framework is then reshaped by:
Once reshaping is complete, the tissues are redraped, and incisions are closed with dissolvable sutures inside the nose and removable sutures externally. A small splint is placed on the nose to minimize swelling and maintain structural integrity during healing. Internal soft packing may be used to support the nasal septum.
After surgery, you will be monitored in a recovery area until you are ready for discharge. Most patients experience minimal pain, which can be managed with prescribed medications. While nasal packing is rarely needed, initial swelling and limited breathing through the nose are common due to temporary internal splints and swelling.
What to Expect:
Postoperative Instructions
To ensure optimal healing, follow these guidelines:
Day of Surgery:
First 72 Hours:
First Two Weeks:
By following these guidelines and maintaining open communication with our team, you can achieve a smoother recovery and optimal results from your rhinoplasty procedure.
To learn more or schedule an appointment, contact us today.
You may be up and around as tolerated but expect to tire more quickly than usual.
Use nasal saline sprays (2-3 sprays in each nostril) at least three times daily to moisturize your nose for the first 2 weeks after surgery.
You will be congested due to the swelling from surgery and will likely need to breathe through your mouth.
You will come into the office for a post-operative check-up, removal of the splint on your nose, and removal of any sutures that you may have.
No alcohol for the first 7 days after surgery, which can increase bruising and swelling.
Your swelling and bruising will gradually fade over this time period.
You will come in for another post-operative check-up at 4-6 weeks, sooner if you are having any questions or concerns.
Eyeglasses should be avoided for the first 4 weeks after surgery until the bones have had adequate time to set in place.
You may apply makeup to conceal bruising, but be sure to avoid anywhere near the incision lines for at least 10 days after surgery.
Rest and good nutrition are important healing factors, especially during the first 6 weeks. Avoid all contact sports and other potential traumatic activities for the first 6 weeks after surgery.
Some degree of swelling may persist for up to 3 months after surgery.
Numbness and tingling around the surgical site are common occurrences. If they do occur, they will gradually subside over several months.
If you need to sneeze in the postoperative period, please leave your mouth open and let the rush of air come out of your mouth.
No nose blowing or straining for two weeks after this surgery unless otherwise directed by your physician.
It is a good idea to use two sprays of saline in each nostril at least four times per day following this surgery. This will help prevent large blood clots from forming that may block your breathing and contribute to more postoperative discomfort.
Yes, after this surgery it is normal for the front teeth and the nasal tip to suffer some numbness. The nerve that provides sensation to this area is often transected during the surgery, and it frequently takes up to 6 weeks or more for the sensation to fully recover in this area.
Do not worry if the external cast falls off—it is essentially there as a reminder to be gentle with it and not to hit it. However, the tape that is underneath the cast will remain in place until the first postoperative visit and will continue to hold the structure in the desired location during the postoperative period.
The average amount of time that a patient experiences bloody or blood-tinged mucus drainage from their nostrils after this procedure is about 2 days. However, the range of normal is anywhere from one day to a full week. As long as there is not a steady flow of active bleeding from the nose, then continue to use the nasal “drip pad” provided to you at the time of surgery and the drainage will continue to slow and ultimately stop, almost always within one week.
These thin sheets of plastic are called silastic splints and they are held in place with a suture to keep your septum stable in the postoperative period. The suture and the splints will most likely be removed at your first postoperative visit.
We recommend taking a full week off of work or school to adequately rest and recuperate from your rhinoplasty procedure. We will see you in the clinic one week after your surgery to ensure everything is healing properly and to remove any packing or splints. Depending on your occupation and the ease of your recovery, you may be feeling up to returning to work after that first week. However, you should expect to take it easy for the first two weeks after surgery by avoiding heavy lifting or strenuous exercise, and you should avoid any contact sports for six full weeks.
If you have trouble breathing through your nose, there may be several causes; it’s important to seek out a qualified specialist for an expert evaluation. The nasal turbinates are shelf-like bones located on the walls on each side of the nasal cavity and are covered by mucous membranes. Their function is to warm, moisten, and
If you have trouble breathing through your nose, there may be several causes; it’s important to seek out a qualified specialist for an expert evaluation. The nasal septum is the structure that separates the two nasal passages, provides support to the outside of the nose, and improves airflow dynamics inside the nose. It is made
Most patients seeking a nose job are good candidates for rhinoplasty surgery; however, you should always review the benefits as well as the risks for any procedure with your surgeon. Rapport with your surgeon may be the most critical component when deciding to proceed with any surgery. You want to choose a provider you genuinely
Message Sent!

Dr. Michael Reilly is double board-certified by the American Board of Otolaryngology--Head & Neck Surgery and The American Board of Facial Plastic & Reconstructive Surgery. He specializes in facial plastic surgery and Rhinoplasty.
Follow up appointments:
Medical emergency:
Clinical questions: