3800 Reservoir Rd, 1st Floor Gorman
Washington, DC 20007
6862 Elm St, Suite 800B
McLean, VA 22101
3800 Reservoir Rd, 1st Floor Gorman
Washington, DC 20007
6862 Elm St, Suite 800B
McLean, VA 22101
Message Sent!
Functional Rhinoplasty is surgery that involves modifying the external/outside nasal structures in order to help enhance nasal breathing, which can have beneficial effects on your overall health. Trauma and/or variations in natural nasal anatomy can lead to anatomic causes of nasal obstruction. These anatomic obstructions are often found in combination with underlying causes of nasal lining inflammation, such as chronic allergies and/or sinusitis.
Functional rhinoplasty surgery involves surgical incisions in the nose and nostril area. In some cases, cartilage from the ear or rib is necessary to help provide additional structure to the nose. When this is necessary, surgical cuts in the outer part of the ear are also required. Like with any surgery, complications and unsatisfactory results are possible, but the vast majority of patients achieve great benefits from functional rhinoplasty surgery.
In the office, I will perform an in-depth analysis of the nasal anatomy from frontal, profile, base, and oblique views. I will determine whether there are any areas of collapse or weakness that may be contributing to your difficulty breathing through your nose. I will also typically use a small endoscope to assess the internal anatomy of the nose in order to determine potential internal sources of the obstruction. We will discuss how changes to different areas of your nose may affect the contour and breathing functionality of the nose. With proper analysis, realistic patient expectations and the skills of a qualified surgeon, functional rhinoplasty is a very successful procedure in the vast majority of patients.
The technique involves first accessing the bone and cartilage support of the nose. This is done with a combination of incisions made inside the nose and in the small strip of skin separating the nostrils. Next, the underlying bone and cartilage is repositioned and/or supported to create a stronger structure and/or to correct any post-traumatic deformity that is contributing to nasal obstruction.
Once this work is complete, the skin is then replaced over the new structural frame and the incisions are closed with dissolving sutures both on the inside and outside of the nose. A small plastic splint and/or surgical tape is usually applied to the outside of the nose to minimize swelling and to help maintain the new shape while the nose heals. Soft sheets made of silicone and plastic are often placed inside the nose to maintain stability of the nasal septum (the dividing wall between the two sides of the nasal cavity) during the healing period. These sheets, called splints, are held in place by a single suture and are typically removed about one week after surgery at your first postoperative appointment.
While the vast majority of patients undergo this surgery without complications, there are always risks to surgery. The possible complications of functional rhinoplasty surgery include but are not limited to the following:
Infection, bleeding, swelling, scarring, numbness, skin discoloration, persistent nasal obstruction, palpable and/or visible irregularities, asymmetry, undesirable change to the nasal appearance, and allergic or other negative reactions to one or more of the substances used in the operation. Some complications may result in the need for further surgery.
Upon completion of the surgery, you will be monitored in the post-anesthesia care area (PACU) until you feel well enough for discharge home. This is typically about 2-3 hours after surgery.
The majority of patients experience only mild to moderate pain after this procedure. Most patients will comment that their nasal breathing is limited in the first week after surgery. This is a result of intranasal swelling. As the swelling subsides, your breathing will improve.
After this surgery it is normal for the nose to feel firm and stiff, and even to feel some limitations in mouth movement, specifically smiling, due to swelling in the area. These symptoms typically resolve over the course of 2 weeks.
It is also normal to have some numbness in the front teeth and the nasal tip. The nerve that provides sensation to this area is often transected during the surgery, and it frequently takes up to 6 weeks or more for the sensation to fully recover in this area.
There will be a small dressing under the nostrils called a “drip pad,” which can be replaced as needed when it is saturated. The nurses will provide you with supplies to change this as needed before you are discharged. Try not to change this dressing until the bandage is fully saturated as frequent bandage changes may prolong the period of bleeding after surgery. If there are any external incisions, please apply Vaseline to them at least twice per day to keep them moist.
If there is tape and/or a plastic splint on the outside of the nose, please leave it in place. You may wash around the rest of your face with soap and water as usual, but try not to get the tape wet and/or inadvertently remove the cast. If the cast does come off, you may leave it off.
The majority of patients experience only mild to moderate pain after this procedure. However, analgesic medications are typically given as needed for post operative discomfort. About one-third of patients will be able to manage their pain with just over the counter acetaminophen, about one-third will require some narcotic medication for up to 3-4 days, and another one-third will require narcotic medication for a full week. It is rare for a patient to require any narcotic medication beyond a week after this surgery.
I do not typically use any nasal packing beyond the thin sheets of silicone and plastic called “splints,” which are sutured in place with a single stitch to keep the nasal septum in place and protected during the week after surgery.
A nasal dressing is typically placed underneath the nostril to help collect any drainage of blood or mucous from the nose during the postoperative period. The average amount of time that a patient experiences bloody or blood-tinged mucous drainage from their nostrils after this procedure is about 2-3 days. However, the range of normal is anywhere from one day to a full week. As long as there is not a steady flow of active bleeding from the nose, then continue to use the nasal “drip pad” provided to you at the time of surgery and the drainage will continue to slow and ultimately stop, almost always within one week. Once the nose is no longer draining, the dressing can be removed and does not need to be replaced.
You are not to blow your nose during the 2 weeks after surgery. Instead, nasal saline spray should be used to help decrease the sensation of congestion by clearing any mucous or blood clots that have formed in the nose. I recommend using at least 2 sprays in each nostril a minimum of four times per day after surgery in order to help keep the nose clear. This should be started immediately after surgery, even during the period when the nose is still draining onto the dressing. This will help prevent large blood clots from forming that may block your breathing and contribute to more post-operative discomfort. If you need to sneeze during the 2 weeks after surgery, please do so with your mouth open.
Your face will feel puffy, especially the first day after surgery. Some patients develop swelling and/or bruising around the eyes. This generally subsides in the first 7 days after surgery. Cold compresses will help minimize and reduce the bruising and any discomfort.
Absorbable sutures are generally used inside the nose and do not need removal. Sutures on the outside of the nose are also absorbable, but the visible tips of these sutures may be trimmed at your postoperative visit for appearance reasons.
Most patients are given prescriptions for pain medication, an antibiotic, and an anti-nausea medication to be used after surgery. Some patients are also given a prescription for a steroid pill to reduce the swelling and inflammation from surgery. You will be provided with these prescriptions the day of surgery, which can be filled at our pharmacy while you are in the operating room.
Expect to eat a liquid and soft diet for the first few days after surgery. Chewing may be uncomfortable due to irritation of the masseter muscle that lies below the parotid gland in the cheek. This gradually improves as you heal, and generally you will be able to eat normally the week following surgery.
It is imperative that you follow the postoperative instructions. Keeping your head elevated will minimize swelling. It is important not to blow your nose and to avoid any impact to the nose while the structures inside and out are healing. Activities such as heavy lifting, excessive exertion, sun exposure or any activity that would increase the risk of injury should be avoided. If you wear glasses, you must be careful not to exert excess pressure on the bridge of the nose. Tape and other devices are sometimes used to permit wearing glasses without stressing the area during healing.
Follow-up care is crucial to success in rhinoplasty. Any concerns regarding your postoperative course such as excess bleeding (a continuous stream of blood and/or persistent drainage beyond 3 days), unexpected swelling, fever, or worsening pain should be reported to your surgeon immediately. It is essential that you keep your follow-up appointments with your surgeon. As your healing is being monitored, there may be techniques such as massage, use of nasal sprays or even small injections of cortisone like medications that can further enhance the desired result.
Day of surgery:
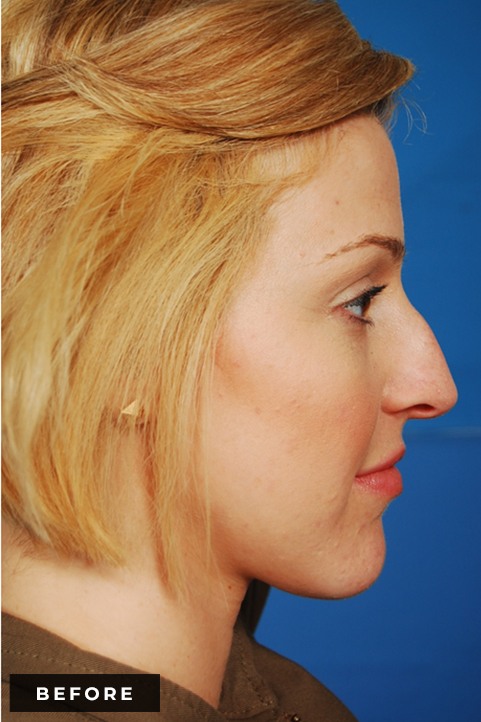
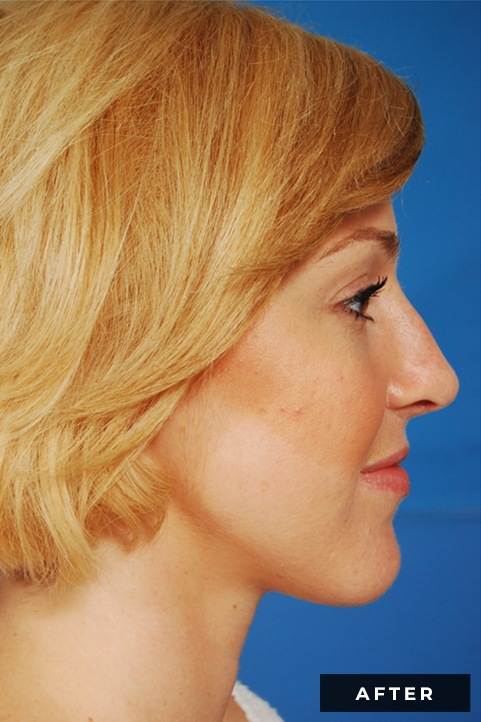

If you have trouble breathing through your nose, there may be several causes; it’s important to seek out a qualified specialist for an expert evaluation. The nasal turbinates are shelf-like bones located on the walls on each side of the nasal cavity and are covered by mucous membranes. Their function is to warm, moisten, and
If you have trouble breathing through your nose, there may be several causes; it’s important to seek out a qualified specialist for an expert evaluation. The nasal septum is the structure that separates the two nasal passages, provides support to the outside of the nose, and improves airflow dynamics inside the nose. It is made
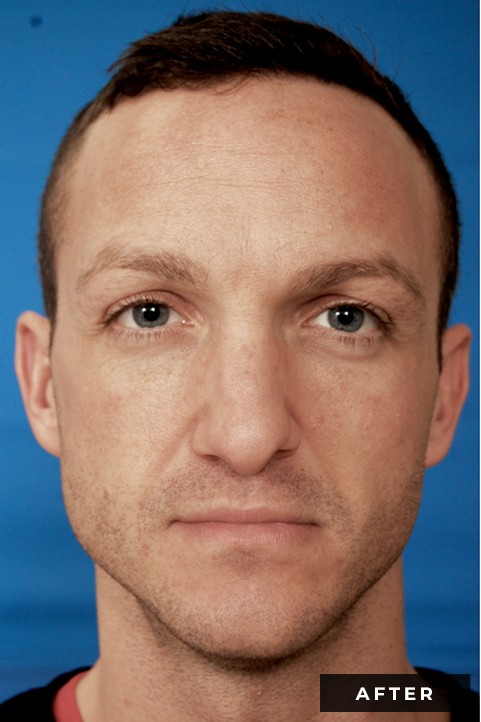
Most patients seeking a nose job are good candidates for rhinoplasty surgery; however, you should always review the benefits as well as the risks for any procedure with your surgeon. Rapport with your surgeon may be the most critical component when deciding to proceed with any surgery. You want to choose a provider you genuinely
Message Sent!

Dr. Michael Reilly is double board-certified by the American Board of Otolaryngology--Head & Neck Surgery and The American Board of Facial Plastic & Reconstructive Surgery. He specializes in facial plastic surgery and Rhinoplasty.
Follow up appointments:
Medical emergency:
Clinical questions: