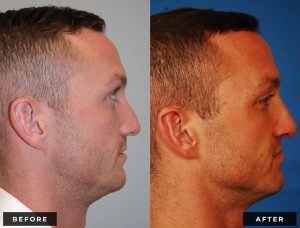
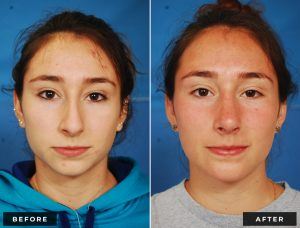
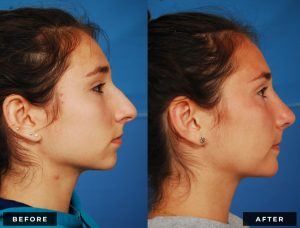
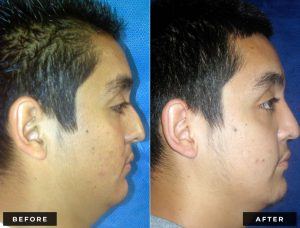
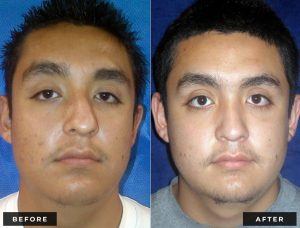
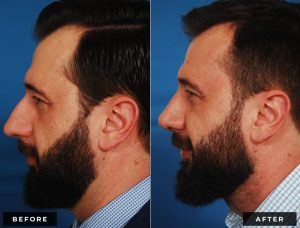
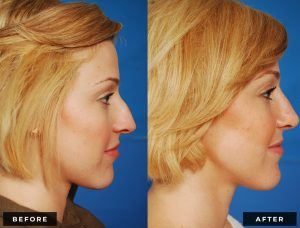
Rhinoplasty, frequently called a “nose job,” is surgery to enhance the form and/or function of the nose.
- 3800 Reservoir Road | 1st Floor Gorman | Washington, DC 20007
- 6862 Elm St | Suite 800B | McLean, VA 22101
- (202) 444-0757
Rhinoplasty
- Home
- Rhinoplasty
At A Glance
Background
Evaluation
Clinical evaluation includes the assessment of your specific nasal anatomy and your desires for change. Dr Reilly will then work with you to create a plan that aligns your goals with potential surgical treatments based on your anatomy.
Pre-op Considerations
Generally, this type of plastic surgery of the nose is not an emergency, but it may help improve your appearance and/or protect your physical health by helping you to breathe more easily.
Surgery
The technique involves incisions inside the nose with or without an incision on the columellar (the small bridge of skin between the nostrils).
Post-op Care
Most patients take one week off work, followed by another week of reduced activity. After 2 weeks, you may resume full activity except contact sports, which must be avoided for 6 weeks.
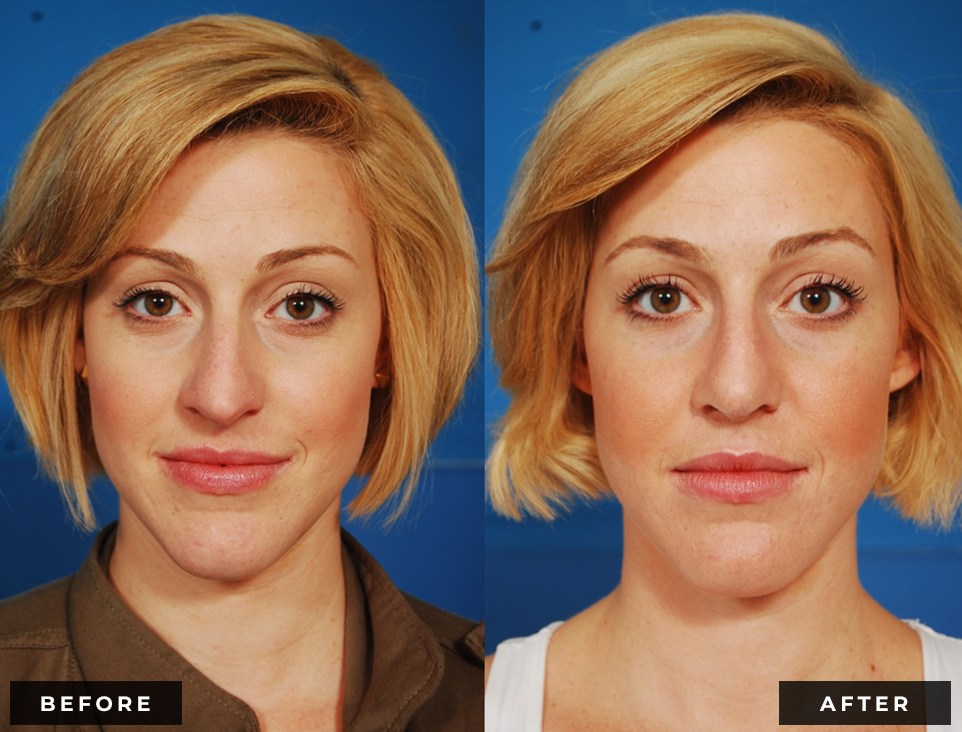
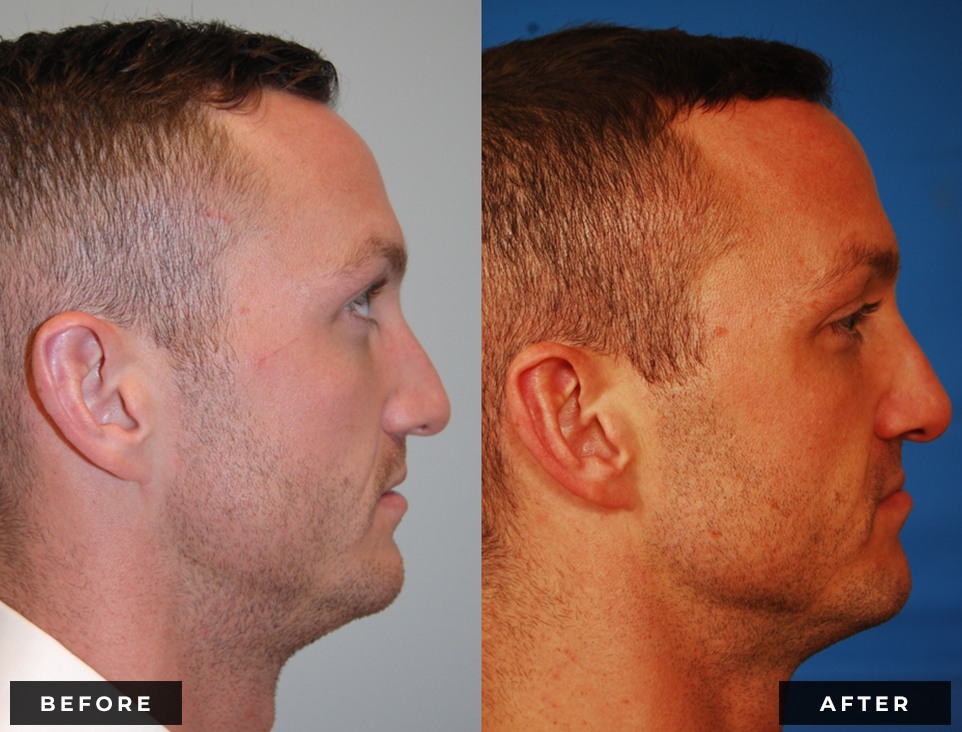
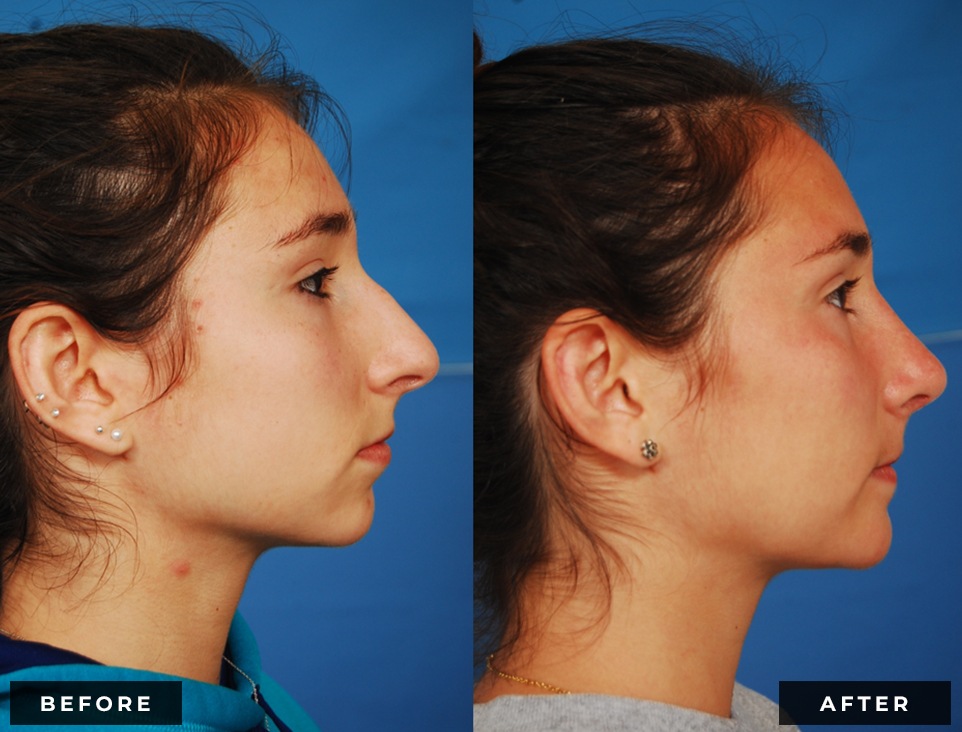
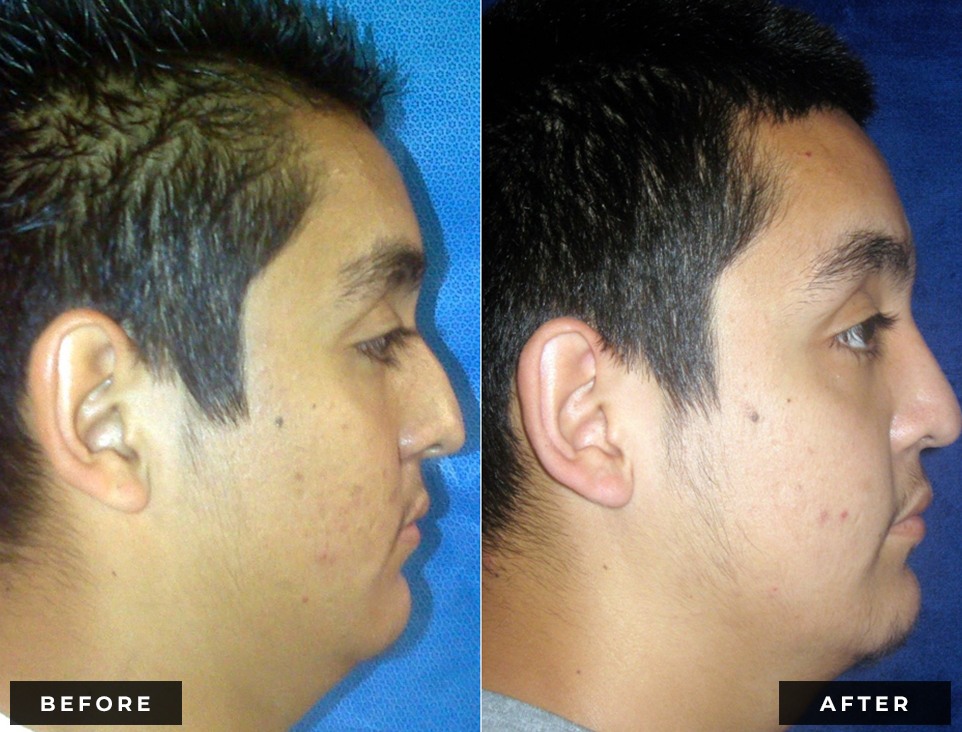
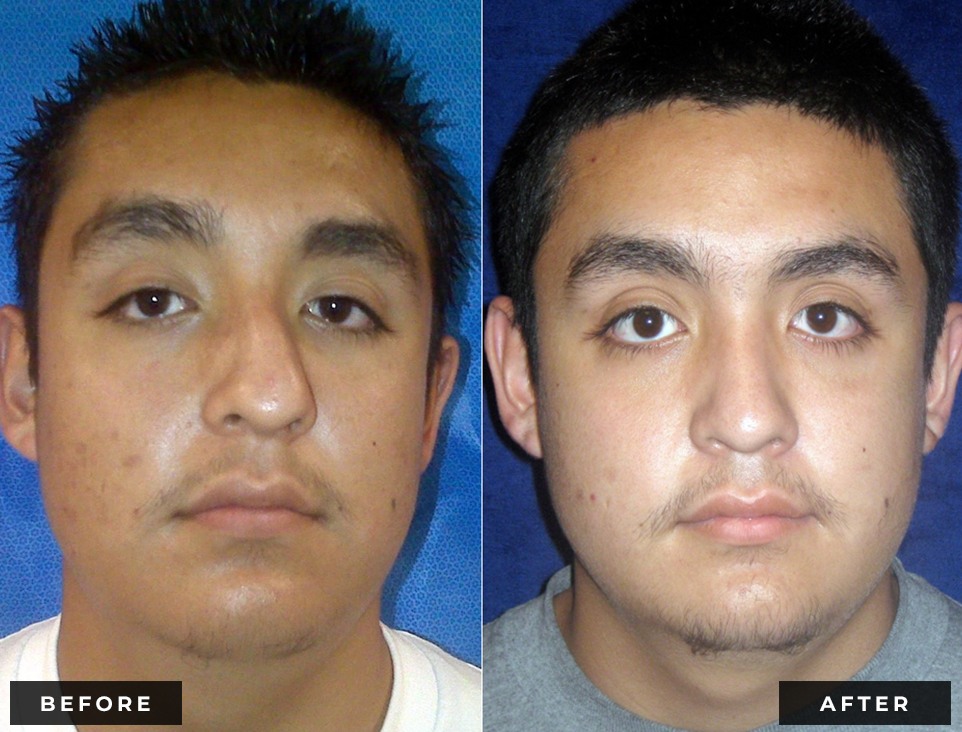
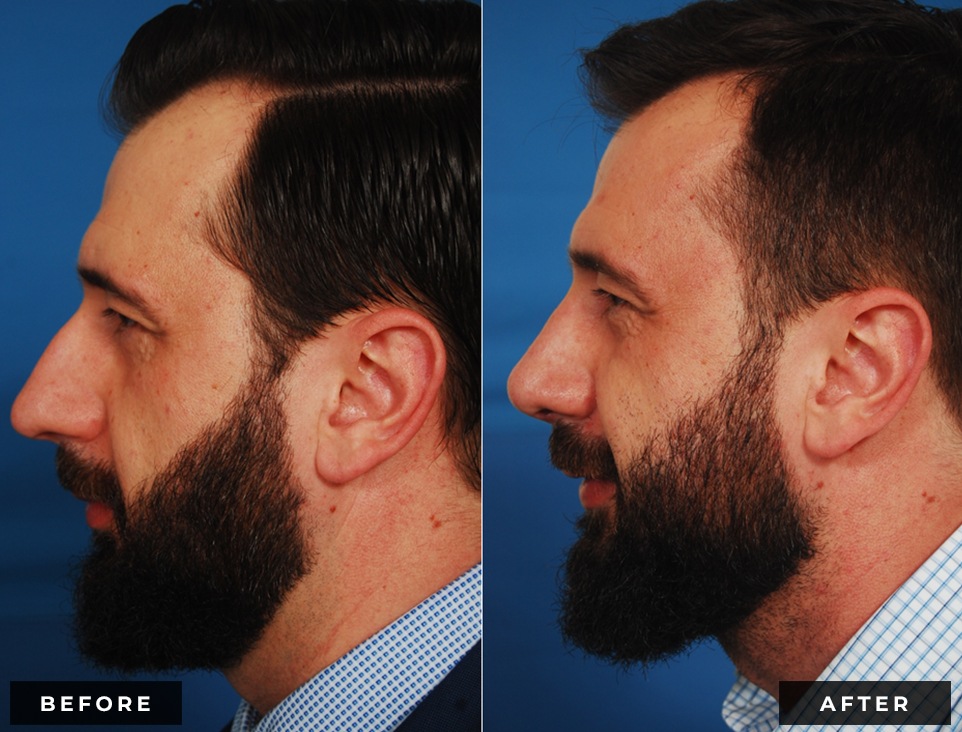
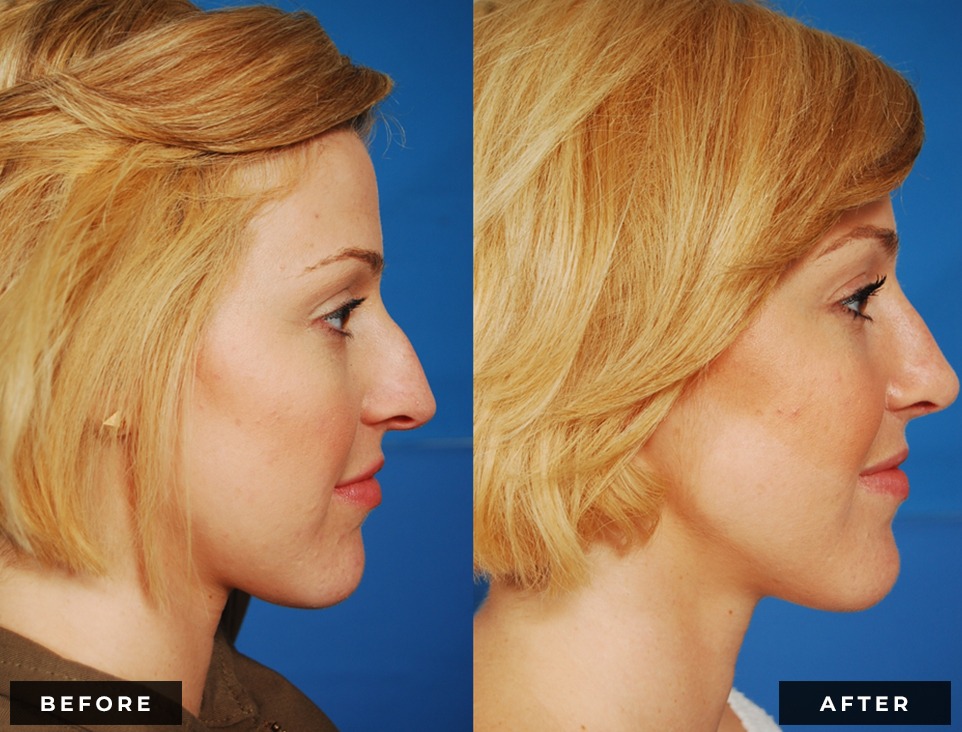
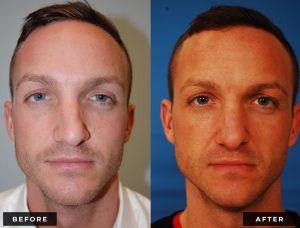
Before and After
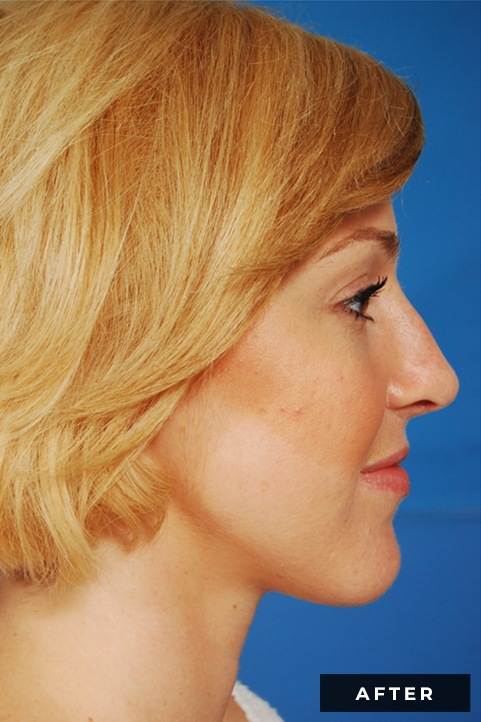

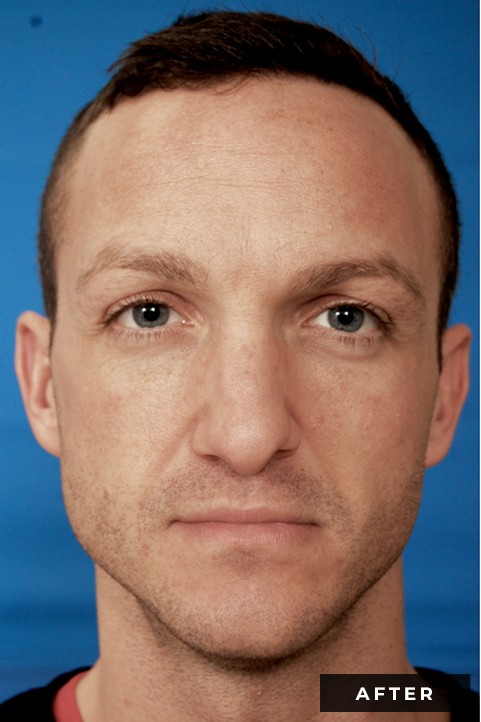
Detailed Information
Background
Rhinoplasty to enhance the appearance of one’s nose is one of the most commonly performed plastic surgeries in the US each year. The nose occupies a central position on the face, and the size and shape of the nose has a great impact on an individual’s appearance.
This procedure can be undertaken for a variety of reasons:
1) Dissatisfaction with the natural nasal appearance and/or the way aging has changed the nose.
2) Distortion of the nose from injury or other trauma.
3) Desire to improve the function of the nose to allow better breathing.
Nasal Evaluation
Dr. Reilly will perform an in-depth analysis of your nose, from frontal, profile, base, and oblique views. He will discuss how changes to different areas of your nose may affect the appearance from each of these perspectives. From the frontal view, the most concerning thing for many patients is when their nose appears widened (either at the base or the tip). Historically, nasal aesthetic ideals dictate that the widest part of the nose should be no wider than the distance between the eyes. The tip of the nose should be approximately half of the overall width of the nasal base. From the side view (profile), the root (top) of the nose should ideally start at the upper eyelashes for women and the upper eyelid crease for men. The tip should project away from the face approximately 55-60% of the total nasal length. The angle between the nose and the upper lip should be maintained between 95-105 degrees for women and 90-100 degrees for me. Viewing the nose from underneath (base view), the nostrils should be symmetrical and oriented in an oblique position relative to the columella (skin between the nostrils). With proper analysis, realistic patient expectations and the skills of a qualified facial plastic surgeon, rhinoplasty is a very rewarding procedure for both patient and surgeon alike.
Pre-operative Considerations
Rhinoplasty is an operation to improve the appearance and/or function of your nose. This surgery involves incisions inside nostril area with or without an incision in the small bridge of skin between the nostrils (columella). In some cases, cartilage from the ear is necessary to help rebuild the nose. When this is necessary, surgical cuts in the outer part of the ear are also required. Generally, this type of plastic surgery of the nose is not an emergency, but it may help improve your appearance and/or protect your physical health by helping you to breathe more easily.
In the vast majority of patients, the desired aesthetic result is readily achieved. However, the possible complications of rhinoplasty surgery include but are not limited to the following:
Infection, bleeding, swelling, scarring, numbness, skin discoloration, nasal obstruction, palpable and/or visible irregularities, asymmetries, displeasure with the cosmetic outcome, personality changes and mental difficulties following surgery (even if the operation is otherwise successful), and allergic or other negative reactions to one or more of the substances used in the operation.
Insurance does not generally cover surgery that is purely for cosmetic reasons. Any component of the surgery aimed at improving nasal function or correcting any traumatic nasal deformity may be partly or entirely reimbursable. Our team will work with your insurance carrier to help determine your eligibility.
Details of Surgery
The technique involves first accessing the bone and cartilage support of the nose. This is done with a combination of incisions made inside the nose and in the area of skin separating the nostrils. Next, the underlying bone and cartilage is reduced, added to, or changed to create a newly shaped structure.
For example, if the tip of the nose is too large, the cartilage in this area can be reduced and/or modified with sutures. If the bridge of the nose has a “hump,” it can be reduced in size and contour. For areas of the nose that are too small, cartilage or soft tissue grafts can be placed to create better proportions. The angles of the nose in relation to the upper lip or the forehead can also be altered by further sculpting the nasal support structure.
Once this work is complete, the tissues are then redraped over the new frame and the incisions are closed with dissolving sutures inside the nose and removable sutures on the outside. A small plastic splint is applied to the outside of the nose to minimize swelling and to help maintain the new shape while the nose heals. Soft, absorbent material may be used inside the nose to maintain stability along the dividing wall of the air passages called the septum.
Postoperative Care
Upon completion of the surgery, you will be monitored in the post-anesthesia recovery area until you feel well enough for discharge home. The majority of patients do not experience any significant pain, however, analgesic medications can be given as needed for post operative discomfort. While packing is only very rarely utilized (<2%), most patients will comment that their nasal breathing is limited in the first few days after surgery. This is a result of intranasal swelling and thin sheets of plastic that are used to maintain stability in the immediate postoperative period. As the swelling subsides, the breathing improves. Your face will feel puffy,especially the first day after surgery. Some patients develop swelling and/or bruising around the eyes. This generally subsides in the 5-7 days after surgery. Cold compresses will help minimize and reduce the bruising and any discomfort. Absorbable sutures are generally used inside the nose and do not need removal. Any external sutures, if required, are removed in 5-8 days. Nasal dressings and splints are also removed at 5-10 days after surgery.
It is imperative that you follow your surgeon’s post operative instructions:
1. Keep your head elevated will minimize swelling.
2. Do not to blow your nose and avoid any impact to the nose while the structures inside and out are healing.
3. Heavy lifting, excessive exertion, sun exposure or any activity that would increase the risk of injury should be avoided for at least 2 weeks after surgery.
4. If you wear glasses, you must be careful not to exert excess pressure on the bridge of the nose. Tape and other devices are sometimes used to permit wearing glasses without stressing the area during healing.
5. Follow-up care is crucial to success in rhinoplasty. It is essential that you keep your follow-up appointments with your surgeon. As your healing is being monitored, there may be techniques such as massage, use of nasal sprays or even small injections of cortisone like medications that can further enhance the desired result.
Post-Operative Recovery Timeline
Day of surgery:
Arrange for someone to stay with you for the first 24 hours.
Go to bed and rest, lying on your back, with your head elevated with 2-3 pillows. You should be lying at a 45 degree angle for the first night after surgery.
You may be up and around and able to go to the bathroom. You will be able to eat a light meal with assistance.
Take medication as directed.
Some swelling, bruising and tightness of the nasal splint are normal occurrences.
Place ice packs on the nose the first 48 hours (on for 20 minutes, then off for 20 minutes).
You should expect to have some bloody mucus from your nose for up to 72 hours after surgery. This will be cared for by placing a “drip pad” under your nose to catch the mucous. This will likely need to be changed every 2-3 hours until the mucous stops.
If you have an active nosebleed (continuous stream of blood), you should lean forward and squeeze the tip of your nose with moderate pressure for 10 minutes. If the nose continues to bleed, you should come to the office/ED to be seen immediately as you may require packing.
NO heavy lifting for 10 days after surgery. No nose picking and/or nose blowing for 14 days after surgery.
You may be up and around as tolerated but expect to tire more quickly than usual.
Use nasal saline sprays (2-3 sprays in each nostril) at least three times daily to moisturize your nose for the first 2 weeks after surgery.
You will be congested due to the swelling from surgery and will likely need to breathe through your mouth.
You will come into the office for a post-operative check-up, removal of the splint on your nose, and removal of any sutures that you may have.
No alcohol for the first 7 days after surgery, which can increase bruising and swelling.
Your swelling and bruising will gradually fade over this time period.
You will come in for another post-operative check-up at 4-6 weeks, sooner if you are having any questions or concerns.
Eyeglasses should be avoided for the first 4 weeks after surgery until the bones have had adequate time to set in place.
You may apply makeup to conceal bruising, but be sure to avoid anywhere near the incision lines for at least 10 days after surgery.
Rest and good nutrition are important healing factors, especially during the first 6 weeks. Avoid all contact sports and other potential traumatic activities for the first 6 weeks after surgery.
Some degree of swelling may persist for up to 3 months after surgery.
Numbness and tingling around the surgical site are common occurrences. If they do occur, they will gradually subside over several months.
FAQ
What do I do if I have to sneeze?
If you need to sneeze in the postoperative period, please leave your mouth open and let the rush of air come out of your mouth.
When Can I blow my nose?
No nose blowing or straining for two weeks after this surgery unless otherwise directed by your physician.
How and when do I use the saline spray?
It is a good idea to use two sprays of saline in each nostril at least four times per day following this surgery. This will help prevent large blood clots from forming that may block your breathing and contribute to more postoperative discomfort.
Is it normal for my teeth to be numb?
Yes, after this surgery it is normal for the front teeth and the nasal tip to suffer some numbness. The nerve that provides sensation to this area is often transected during the surgery, and it frequently takes up to 6 weeks or more for the sensation to fully recover in this area.
What do I do if the cast on the outside of my nose falls off?
Do not worry if the external cast falls off—it is essentially there as a reminder to be gentle with it and not to hit it. However, the tape that is underneath the cast will remain in place until the first postoperative visit and will continue to hold the structure in the desired location during the postoperative period.
How much bleeding from my nose is normal?
The average amount of time that a patient experiences bloody or blood-tinged mucus drainage from their nostrils after this procedure is about 2 days. However, the range of normal is anywhere from one day to a full week. As long as there is not a steady flow of active bleeding from the nose, then continue to use the nasal “drip pad” provided to you at the time of surgery and the drainage will continue to slow and ultimately stop, almost always within one week.
What is the plastic I can see and/or feel inside my nose?
These thin sheets of plastic are called silastic splints and they are held in place with a suture to keep your septum stable in the postoperative period. The suture and the splints will most likely be removed at your first postoperative visit.
Please call (202) 444-0757
Or contact us via email form below
-
Get directions to Dr. Reilly
-
Call for an appointment!
About Us
Dr. Michael Reilly is double board-certified by the American Board of Otolaryngology--Head & Neck Surgery and The American Board of Facial Plastic & Reconstructive Surgery. He specializes in facial plastic surgery and Rhinoplasty.
Follow up appointments:
Medical emergency:
Clinical questions: